Anesthesia Essentials: A Virtual Training Program for Safer Veterinary Anesthesia
Anesthesia Essentials is a structured 12-hour course designed to improve patient safety, team confidence, and anesthetic outcomes.
- Key Features:
- Virtual, asynchronous, self-paced course
- Designed for veterinarians, technicians, and nursing staff
- Ideal for hospitals and organizations aiming to standardize practices and manage risk
- Reduces training burden and bottlenecks, ensuring in-person training is focused and effective
- Applicable to general practice and referral settings
- Focused on real-world decision-making, not just theory
- Built from specialist-level expertise in veterinary anesthesia
🧠 Module 1: Introduction to Safe Anesthesia and Risk Management (1.5 hours)
- Understanding anesthesia risk and the sedation–anesthesia continuum
- Patient risk assessment and ASA physical status classification
- Communicating anesthetic risk and expectations effectively with clients
- Human factors and James Reason’s Swiss Cheese Model of accident causation
- Situational awareness, workload, and task saturation during anesthesia
- Communication strategies that improve patient safety and team coordination
- Psychological safety and speaking up about concerns
- Cognitive aids, checklists, and standardized safety procedures
- The sterile induction rule and reducing distractions during critical moments
- Post-incident debriefing, root cause analysis, and systems improvement
- Practical strategies to strengthen anesthesia safety in everyday clinical practice
⚙️ Module 2: Anesthesia Machines and Equipment (2 hours)
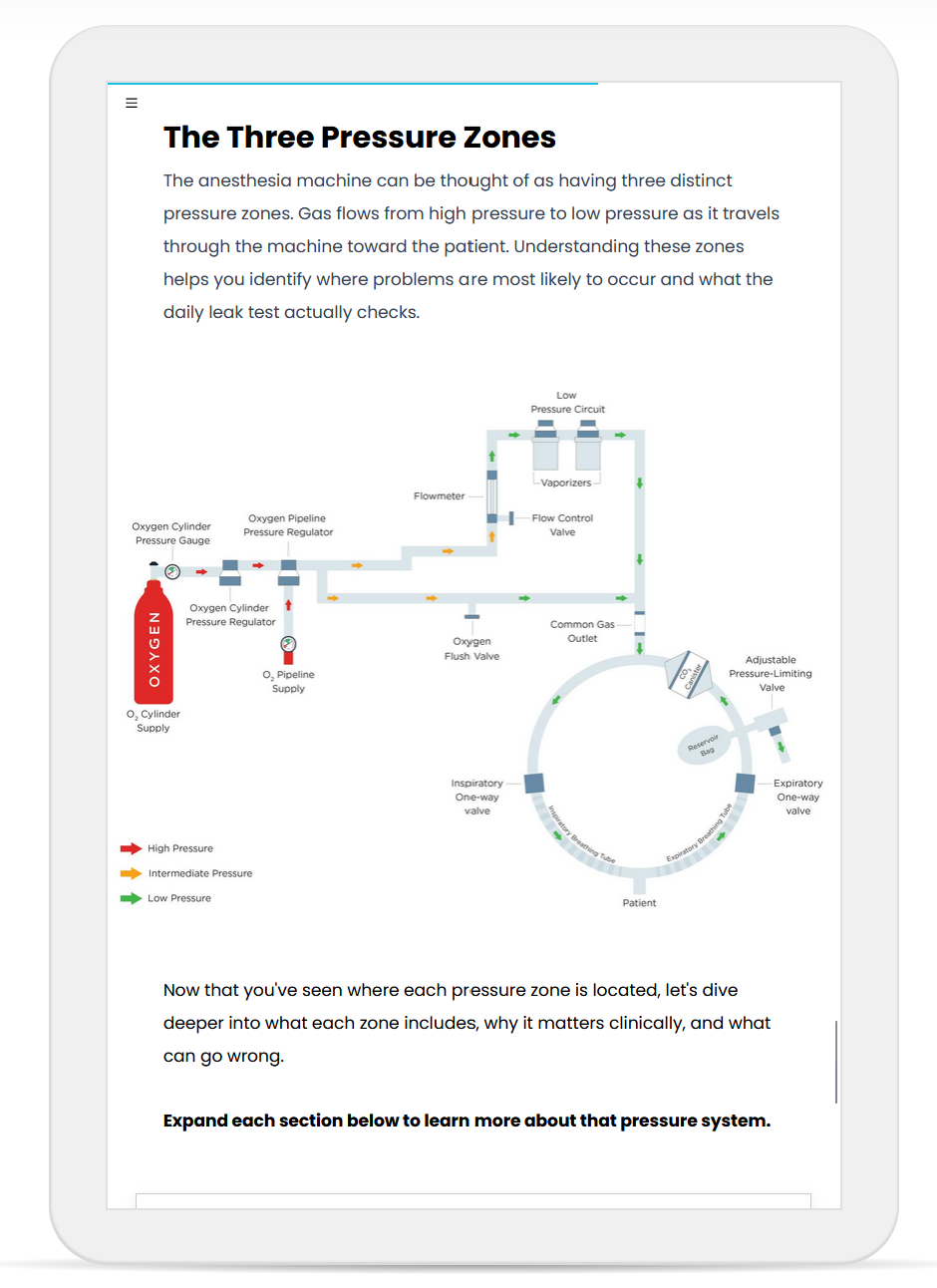
- Understanding the purpose and function of the anesthesia machine
- Oxygen sources, pressure regulators, flowmeters, and vaporizers
- Circle systems, non-rebreathing circuits, and breathing circuit selection
- Carbon dioxide absorption, dead space, and rebreathing physiology
- Common gas outlet (CGO/ACGO) systems and oxygen flush valve safety
- Scavenging systems and waste anesthetic gas exposure
- Daily machine safety checks and leak testing
- Equipment troubleshooting and recognition of common machine faults
- Practical anesthesia workspace setup and preparation
💉 Module 3: Designing an Anesthetic Plan (2 hours)
- The goals of anesthesia and principles of balanced anesthesia
- Major classes of anesthetic and analgesic drugs used in small animal practice
- Opioids, sedatives, induction agents, inhalants, and adjunctive drugs
- Receptor pharmacology, potency, efficacy, and drug interactions
- Patient-specific anesthetic planning based on temperament, disease, and procedure
- Fluid therapy fundamentals and supportive care during anesthesia
- Equipment preparation, airway planning, and warming strategies
- Anticipation of complications and contingency planning
- Building practical, flexible anesthetic protocols rather than memorizing “cookbook” recipes
📋 Module 4: Preparing Patients for Anesthesia and Induction of Anesthesia (1.5 hours)
- Why pre-anesthetic preparation is critical for patient safety
- Medical history, physical examination, and anesthesia-focused patient assessment
- Identifying anesthetic risk factors and comorbidities
- ASA physical status classification and procedural risk assessment
- Breed-specific anesthetic considerations, including brachycephalic patients
- Selection and interpretation of pre-anesthetic diagnostics
- Fasting guidelines, medication management, and client communication
- Preparation of monitoring equipment, airway supplies, and emergency drugs
- Safe anesthesia induction principles, pre-oxygenation, and airway management
- Structured induction workflow, intubation preparation, and transition into maintenance anesthesia
📈 Module 5: Monitoring Anesthetized Patients (2 hours)
- Goals of anesthetic monitoring and goal-directed anesthesia
- Continuous monitoring during induction, maintenance, and recovery
- ECG, blood pressure, pulse oximetry, capnography, and temperature monitoring
- Interpretation of physiologic trends rather than isolated values
- Physical signs of anesthetic depth and patient assessment
- Understanding monitor limitations, artifacts, and troubleshooting abnormal readings
- The anesthesia record as a patient safety and communication tool
- Early recognition of anesthetic complications and physiologic instability
- Integrating monitoring data into clinical decision-making
🚨 Module 6: Introduction to Anesthetic Complications and Troubleshooting (2 hours)
- A structured approach to anesthetic troubleshooting and crisis management
- Recognize → interpret → respond: systematic decision-making under anesthesia
- Cardiovascular complications including hypotension, hypertension, bradycardia, and arrhythmias
- Respiratory complications including hypoventilation, airway obstruction, and hypoxemia
- Thermoregulation, hypothermia, and metabolic disturbances
- Understanding the physiologic mechanisms behind common anesthetic abnormalities
- Troubleshooting monitoring changes and identifying root causes
- Early intervention strategies and prevention of crisis escalation
- Pattern recognition and systems-based thinking during anesthetic complications
🌅 Module 7: Recovering Patients from Anesthesia (1 hour)
- Why recovery is one of the highest-risk phases of anesthesia
- Airway protection, oxygenation, and ventilation during recovery
- Safe extubation criteria and endotracheal tube management
- Recovery monitoring protocols and continuation of physiologic support
- Recognition and management of airway obstruction, hypoventilation, hypoxemia, and dysphoria
- Preparation for recovery complications and emergency re-intubation
- Pain assessment and patient comfort during recovery
- Recovery staffing, communication, and patient handoff procedures
- Creating structured recovery systems that improve patient safety
What Your Team Will Gain
- Improved anesthetic safety and reduced complications
- Greater confidence in monitoring and clinical decision-making
- Standardized safety protocols across your practice
- Earlier detection of complications before they become critical events
- A safety culture that expands beyond anesthesia
Format & Delivery
- On-demand, self-paced learning
- High-quality animations and visual explanations
- Case-based interactive content
- Designed for team-wide implementation
- Annual recertification and focused review of key safety concepts
Additional Courses in Development
- Anesthesia Ventilators
- Equine Anesthesia
- Exotic Animal Anesthesia
- Veterinary Pain Management
- Patient Safety Systems for Hospital Managers